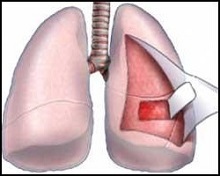
 Pleurisy is an inflammation of the pleura with the formation of a fibrous plaque on its surface or effusion inside it. Appears as an accompanying pathology or as a consequence of various diseases.
Pleurisy is an inflammation of the pleura with the formation of a fibrous plaque on its surface or effusion inside it. Appears as an accompanying pathology or as a consequence of various diseases.
Pleurisy is an independent disease (primary pleurisy), but more often it is the consequences of acute and chronic inflammatory processes in the lungs (secondary pleurisy). Divide into dry, otherwise known as fibrinous, and effusive (serous, serous-fibrinous, purulent, hemorrhagic) pleurisy.
Often pleurisy is one of the symptoms of systemic diseases (oncology, rheumatism, tuberculosis). However, vivid clinical manifestations of the disease often cause doctors to exhibit pleurisy at the forefront, and already by its presence to find out the true diagnosis. Pleurisy can occur at any age, many of them remain unrecognized.
Causes
Why does lung pleurisy occur, what is it, and how to treat it? Pleurisy is a disease of the respiratory system, with its development inflamed visceral (pulmonary) and parietal (parietal) the pleura - a connective tissue membrane that covers the lungs and the inner surface of the chest.
Also, pleurisy between the pleura (in the pleural cavity) can be deposited liquids, such as blood, pus, serous or putrefactive exudate. The causes of pleurisy can be conditionally divided into infectious and aseptic or inflammatory (non-infectious).
Infectious causespleurisy lungs include:
- bacterial infections (pneumococcus, staphylococcus),
- fungal lesions (blastomycosis, candidiasis),
- syphilis,
- typhoid fever,
- tularemia,
- tuberculosis,
- trauma of the chest,
- surgical interventions.
Causes of noncommunicablepleurisy of the lungs are as follows:
- malignant tumors of pleural sheets,
- metastasis in the pleura (with breast cancer, lung, etc.),
- connective tissue lesions of diffuse nature (systemic vasculitis, scleroderma, systemic lupus erythematosus), lung infarction,
- PE.
Factors that increase the risk of developmentpleurisy:
- stress and overwork;
- supercooling;
- unbalanced food, poor in nutrients;
- hypokinesia;
- medicinal allergies.
The course of pleurisymay be:
- acute up to 2-4 weeks,
- subacute from 4 weeks to 4-6 months,
- chronic, more than 4-6 months.
The microorganisms enter the pleural cavity in different ways. Infectious agents can penetrate by contact, through blood or lymph. Direct hit them occurs with injuries and injuries, during surgery.
Dry Pleurisy
With dry pleurisy, there is no liquid in the pleura, fibrin acts on its surface. Basically, this form of pleurisy precedes the development of exudative.
Dry pleurisy is often a secondary disease in many diseases of the lower respiratory tract and intrathoracic lymph nodes, malignant neoplasms, rheumatism, collagenoses and some viral infections.
Tuberculous pleurisy
Recently, the incidence of tuberculous pleurisy has increased, which occurs in all forms: fibrotic, exudative and purulent.
In almost half of cases, the presence of dry pleurisy indicates that the body has a latent form of the tuberculosis process. By itself, pleural tuberculosis is rare, and for the most part fibrous pleurisy is a response to tuberculosis of the lymph nodes or lungs.
Tuberculous pleurisy, depending on the course of the disease and its features, is divided into three varieties: perifocal, allergic and tuberculosis of the pleura proper.
Purulent pleurisy
Purulent pleurisy causes such microorganisms as pathogenic staphylococci, pneumococci, streptococci. In rare cases, these are Proteus, Escherichian sticks. As a rule, purulent pleurisy develops after exposure to one type of microorganism, but it happens that the disease causes a whole association of microbes.
Symptoms of purulent pleurisy. The course of the disease differs according to age. In infants of the first three months of life, purulent pleurisy is very difficult to recognize, as it disguises itself under the general symptoms associated with umbilical sepsis, pneumonia caused by staphylococci.
From the side of the disease, the chest becomes convex. Also, there is a lowering of the shoulder, insufficient mobility of the arm. Older children experience standard symptoms of total pleurisy. You can also note a dry cough with phlegm, sometimes even with pus - with a breakthrough abscess of the pleura in the bronchi.
Closed pleurisy
Purulent pleurisy is one of the most severe forms of pleurisy, in which the splicing of pleural sheets leads to the accumulation of a pleural extrudate.
This form develops as a result of prolonged inflammatory processes in the lungs and pleura that lead to numerous spikes and delimit the exudate from the pleural cavity. Thus, the effusion accumulates in one place.
Exudative pleurisy
Distinguishes exudative pleurisy by the presence of fluid in the cavity of the pleura. It can be formed as a result of a chest injury with bleeding or hemorrhage, lymph flow.
By the nature of this fluid, the pleurisy is divided into serous-fibrinous, hemorrhagic, chyleous and mixed. This fluid, often of unknown origin, is called an effusion, which is also capable of restraining the movement of the lungs and making breathing difficult.
Symptoms of pleurisy
In the case of pleurisy, symptoms may differ depending on how the pathological process proceeds - with exudate or without it.
Dry pleurisy is characterized by the following symptoms:
- Stitching pain in the chest, especially when coughing, deep breathing and sudden movements,
- forced position on the diseased side,
- superficial and sparing breath, while the affected side visually lags behind in the breath,
- when listening - noise of friction of the pleura, weakening of breathing in the zone of fibrin deposits,
- fever, chills and intense sweating.
With exudative pleurisy, the clinical manifestations are somewhat different:
- dull pain in the affected area,
- dry painful cough,
- a strong lag in the affected area of the chest in breathing,
- a feeling of heaviness, shortness of breath, bulging of gaps between the ribs,
- weakness, fever, severe chills and profuse sweat.
The most severe course is noted with purulent pleurisy:
- high body temperature;
- severe chest pain;
- chills, aches all over the body;
- tachycardia;
- earthy shade of skin;
- weight loss.
If the course of pleurisy acquires a chronic character, the lungs form cicatricial changes in the form of pleural adhesions, which prevent the full spreading of the lung. Massive pneumofibrosis is accompanied by a decrease in the perfusion volume of lung tissue, thereby aggravating the symptoms of respiratory failure.
Complications
The outcome of pleurisy largely depends on its etiology. In cases of persistent pleurisy, further development of the adhesion process in the pleural cavity, the infection of the interlobar cracks and pleural cavities, the formation of massive moles, the thickening of the pleural sheets, the development of pleurosclerosis and respiratory failure, the limitation of the movement of the dome of the diaphragm.
Diagnostics
Before determining how to treat pleurisy of the lungs, it is worth to go through the examination and determine the causes of its occurrence. In the clinic, the following examinations are used to diagnose pleurisy:
- examination and questioning of the patient;
- clinical examination of the patient;
- X-ray examination;
- blood test;
- analysis of pleural effusion;
- microbiological study.
Diagnosis of pleurisy as a clinical condition usually presents no special difficulties. The main diagnostic difficulty in this pathology is to determine the cause that caused inflammation of the pleura and the formation of pleural effusion.
How to treat pleurisy?
When symptoms of pleurisy appear, treatment should be comprehensive and aimed primarily at eliminating the main process that led to its development. Symptomatic treatment is intended to anesthetize and speed up the resorption of fibrin, to prevent the formation of extensive splints and fusions in the pleural cavity.
At home, only patients with diagnosed dry (fibrinous) pleurisy are eligible for treatment, all other patients should be hospitalized for examination and selection of an individual treatment regimen for lung pleurisy.
The profile department for this category of patients is the therapeutic department, and patients with purulent pleurisy and empyema pleura require specialized treatment in a surgical hospital. Each of the forms of pleurisy has its own peculiarities of therapy, but in any type of pleurisy, etiotropic and pathogenetic direction in treatment is shown.
So,with dry pleurisy the patient is assigned:
- Pain relief is prescribed for analgesic drugs: analgin, ketones, tramadol if ineffectiveness of these funds, the introduction of narcotic analgesics is possible in a hospital.
- Effective warming semi-alcohol or camphor compresses, mustard plasters, iodide mesh.
- Prescribe drugs that suppress cough - sinecode, kodelak, libeksin.
- Since the root cause is most often tuberculosis, after confirmation of the diagnosis of tuberculous pleurisy in the TB dispensary, specific treatment is carried out.
If the pleurisy is exudative with a lot of effusion, make a pleural puncture for its evacuation or drainage. At a time, no more than 1.5 liters of exudate is pumped out, so as not to provoke cardiac complications. With purulent pleurisy, the cavity is washed with antiseptics. If the process has become chronic, resort to pleurectomy - surgical removal of the pleura to prevent relapse. After resorption of exudate, patients are prescribed physiotherapy, physiotherapy exercises, respiratory gymnastics.
In case of acute tuberculous pleurisy, preparations such as isoniazid, streptomycin, ethambutol or rifampicin may be included in the complex. The course of treatment of tuberculosis itself takes about a year. With parapnevognicheskom pleuritis, the success of treatment depends on the selection of antibiotics based on the sensitivity of pathological microflora to them. In parallel, immunostimulatory therapy is prescribed.

How to choose probiotics for the intestine: a list of drugs.

Effective and inexpensive cough syrups for children and adults.
Modern non-steroidal anti-inflammatory drugs.

Review of tablets from the increased pressure of the new generation.
 Antiviral drugs are inexpensive and effective.
Antiviral drugs are inexpensive and effective.



